Medical Billing Outsourcing Market Trends: Healthcare Digitization, Revenue Cycle Optimization & Forecast to 2034
Expanding healthcare infrastructure, rising demand for automated billing solutions, and growing complexity of insurance claims are driving the global Medical Billing Outsourcing Market.
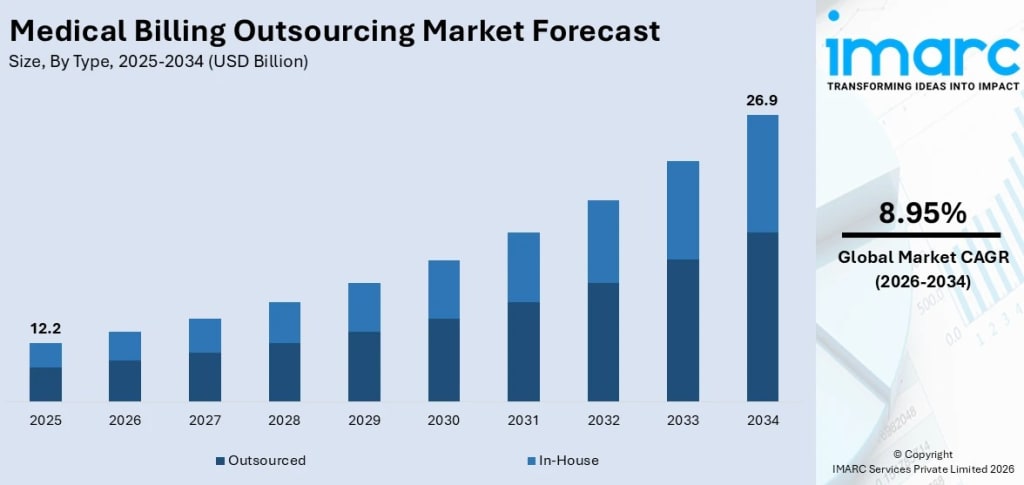
Medical billing sounds like a back-office function — and for a long time, most healthcare organisations treated it that way. That is changing fast. Denied claims, coding errors, regulatory non-compliance, and missed revenue are now material financial risks for hospitals and physician practices alike, and the internal teams built to manage them are simply not keeping up with the pace of regulatory change, payer complexity, and technology demands. Outsourcing the entire revenue cycle has shifted from a cost-cutting move to a strategic imperative. According to IMARC Group, the global medical billing outsourcing market size reached USD 12.2 Billion in 2025. Looking forward, IMARC Group expects the market to reach USD 26.9 Billion by 2034, exhibiting a growth rate (CAGR) of 8.95% during 2026–2034. North America exhibits a clear dominance, accounting for the largest medical billing outsourcing market share.
The market is structured across type, service line, and end-use. By type, outsourced billing dominates — and by a significant margin — because specialist firms bring coding expertise, compliance infrastructure, and AI-driven billing technology that most healthcare providers simply cannot replicate in-house at comparable cost. Front-end services lead by service line, covering the critical first steps of patient registration, insurance verification, and charge capture where billing accuracy is fundamentally established. Hospitals are the largest end-use segment, reflecting their sheer transaction volume, multi-specialty coding complexity, and the enormous financial consequences of revenue cycle inefficiency at that scale.
Get a Sample Report for Actionable Market Insights
Medical Billing Outsourcing Market Growth Drivers:
• Escalating Healthcare Complexity Making In-House Billing Increasingly Unmanageable
The US healthcare billing environment has become genuinely difficult to manage internally. With thousands of ICD-10 codes, constantly shifting payer rules, and value-based care models layered on top of traditional fee-for-service, even experienced in-house teams struggle to maintain accuracy. The average hospital claim denial rate sits between 5% and 10%, and each denied claim costs roughly USD 25 to rework — at high-volume institutions, that adds up to millions in annual administrative waste. Outsourced billing companies invest continuously in coder training, regulatory updates, and AI-assisted claim scrubbing tools that individual hospitals simply cannot justify replicating at equivalent scale internally.
• Rising Cybersecurity Threats Pushing Healthcare Providers Toward Specialist Data Handlers
Healthcare data is among the most targeted in any industry — and the financial and reputational consequences of a breach are severe. IBM's Cost of a Data Breach report consistently ranks healthcare as the highest-cost sector for breach incidents, with average costs exceeding USD 10 million per event. Medical billing outsourcing firms specialise in the security infrastructure that patient financial data demands — HIPAA-compliant encryption, role-based access controls, intrusion detection, and regular audits. For hospitals and physician practices that lack dedicated cybersecurity teams, outsourcing billing to a specialist firm is often the most reliable way to meet data protection obligations while keeping operational focus on clinical care.
• Telemedicine Expansion Creating New Billing Complexity That Specialist Firms Are Built to Handle
The explosive growth of telehealth has introduced billing challenges that most in-house teams were never set up to manage. Remote consultations span state lines, involve varied insurance coverage rules, and require specific billing codes that differ from in-person visit equivalents. The US telehealth market served approximately 116 million patients, and billing each encounter correctly requires navigating a patchwork of payer-specific policies that change frequently. Outsourced billing companies that specialise in telehealth revenue cycles bring both the regulatory knowledge and the technology infrastructure to handle this complexity accurately — directly protecting provider revenue from the claim denials that frequently follow telehealth billing errors.
Medical Billing Outsourcing Market Trends:
• AI and Automation Transforming Revenue Cycle Management From Reactive to Predictive
The most meaningful shift happening in medical billing outsourcing right now is the move from manual claim processing to AI-driven revenue cycle management. Predictive denial analytics can flag claims likely to be rejected before they are even submitted, allowing billing teams to correct errors proactively. Automated eligibility verification runs in real time rather than at a single point in the patient journey. Natural language processing tools extract billable data from clinical notes with accuracy that rivals expert coders on routine cases. Companies like R1 RCM — formerly Accretive Health — have built their entire competitive position around this technology stack, and it is setting the performance benchmark for the industry.
• Front-End Service Investment Gaining Recognition as the Key to Downstream Revenue Recovery
There is a growing recognition among healthcare CFOs that most billing problems are not really billing problems — they are registration and verification problems that surface weeks later as denied claims. When a patient's insurance is not properly verified at registration, or their demographic information is captured incorrectly, the entire downstream billing cycle is compromised. This insight is driving significant investment in front-end outsourcing services — patient registration, insurance eligibility checks, prior authorisation, and charge capture — because fixing problems at source is far cheaper than working denials after the fact. Outsourced firms specialising in front-end services typically achieve first-pass claim acceptance rates above 95%, directly improving cash flow for provider clients.
• Medical Tourism Driving International Billing Complexity and Outsourcing Demand
Medical tourism is growing substantially, with patients crossing borders for elective procedures, specialist consultations, and treatments unavailable or unaffordable in their home country. Managing billing across international insurance systems, currency conversions, and different regulatory frameworks is a genuinely specialised function. India, Thailand, Mexico, and Turkey are among the leading medical tourism destinations, and the hospitals serving international patients require outsourcing partners that understand cross-border claim submission, foreign insurer relationships, and multi-currency revenue reconciliation. Cerner's USD 375 million acquisition of Kantar Health reflected the broader industry recognition that data and analytics capabilities are becoming central to navigating this kind of complex, multi-jurisdictional healthcare revenue environment.
Recent News and Developments in the Medical Billing Outsourcing Market
• August 2022: R1 RCM Inc. (formerly Accretive Health) announced a strategic agreement with Emergency Physicians Professional Association (EPPA), a physician group delivering emergency medicine and urgent care across Minnesota. The partnership extends R1 RCM's technology-driven revenue cycle management platform to EPPA's operations, improving billing accuracy, claim submission speed, and overall financial performance.
• April 2021: Cerner Corporation announced the USD 375 million cash acquisition of Kantar Health, a global life sciences data and analytics firm. The acquisition was designed to accelerate innovation in life sciences research and improve patient outcomes by combining Cerner's clinical data infrastructure with Kantar's real-world evidence and analytics capabilities.
• 2024: GE Healthcare continued expanding its revenue cycle management solutions portfolio, integrating AI-powered claim analytics and prior authorisation automation tools into its billing platform. The enhancements target hospitals seeking to reduce administrative burden, accelerate reimbursement timelines, and improve first-pass claim acceptance rates across complex multi-payer environments.
• 2024: McKesson Corporation advanced its healthcare technology services offering by deepening integration between its billing infrastructure and electronic health record systems. The initiative targets mid-sized hospital systems and physician groups looking to consolidate their revenue cycle management under a single platform, reducing handoff errors between clinical documentation and billing claim generation.
• 2024: Genpact expanded its healthcare business process outsourcing capabilities with new AI-driven denial management and claims adjudication services. The expansion responds to growing demand from US hospital systems for outsourcing partners that can combine deep billing domain expertise with advanced automation to reduce claim rejection rates and accelerate revenue recovery from outstanding payer balances.
Note: If you require specific details, data, or insights that are not currently included in the scope of this report, we are happy to accommodate your request. As part of our customization service, we will gather and provide the additional information you need, tailored to your specific requirements. Please let us know your exact needs, and we will ensure the report is updated accordingly to meet your expectations.
About the Creator
Rahul Pal
Market research professional with expertise in analyzing trends, consumer behavior, and market dynamics. Skilled in delivering actionable insights to support strategic decision-making and drive business growth across diverse industries.





Comments
There are no comments for this story
Be the first to respond and start the conversation.